The Silent Tax: How Poverty Rewires Your Body and What We Can Do About It
We often discuss poverty in terms of financial constraints, debt, and material scarcity. We discuss lines of unemployment and food deserts. The physiological change that results when survival is a constant, grating weight, however, is the most intimate and terrible cost we seldom discuss. This extends far beyond simply being unable to afford a doctor. It’s about how the very state of being poor, the unrelenting strain of precarious life, completely rewrites your biology, therefore creating a pre-existing condition long before any formal diagnosis. The low-income health challenges we encounter are not just care deficits; they are the body’s weary reaction to a hostile environment.
Why Does Chronic Stress Become a Physical Disease for the Poor?
For the wealthy, stress could be a project deadline or a demanding social calendar—severe but often transient. Stress is a continuous, low-grade thrum that never stops for someone living in poverty. It is the calculation of whether the gas tank will last until payday. It’s the anxiety of a child’s fever because a missed work shift means a missed bill. This is chemical, not mental. The hypothalamic-pituitary-adrenal (HPA) axis, the body’s primary stress-response system, is often activated in a state of constant readiness.
This relentless flood of adrenaline and cortisol is damaging as well as exhausting. It raises blood pressure, damages immune response, encourages visceral fat storage near organs, and changes brain chemistry. The body basically damages itself for tomorrow in an attempt to survive what is seen as an emergency of today. Poverty not only restricts access to healthcare but also actively generates disease from the inside out.
How Does Your Zip Code Dictate Your Lifespan More Than Your Genetic Code?
For chronic disease, the surroundings mandated by poverty are a perfect storm. Consider the real facts. Midnight finds a second-shift employee home in a food desert. Their sole food choices are from a gas station or a fast-food drive-thru—high in salt, sugar, and saturated fats, the exact ingredients that fuel inflammation, diabetes, and heart disease. They reside in an area where parks are not well kept, streets are hazardous, and safe outdoor activity is not provided.
They could dwell in subpar housing with mold triggers for asthma or inadequate insulation, worsening respiratory problems. Living where rent is lowest often directly conflicts with the biological need for clean air, safe surroundings, and wholesome food—an economic choice. This environmental cost is a gradual, incremental poison; hence, if the very planet you can afford to live on is making you ill, inexpensive health care is irrelevant.
What Is the True Cost of Choosing Between a Prescription and a Light Bill?
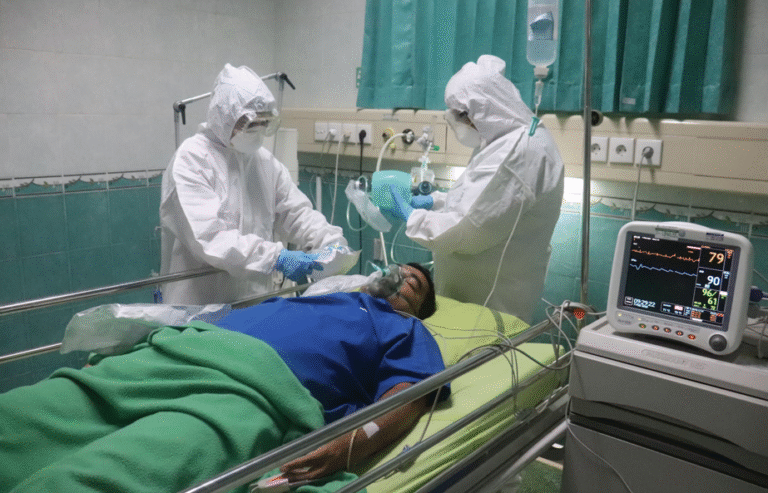
Low-income health challenge in low bedget households’ economic effects of disease generate a vicious spiral nearly impossible to escape. Diabetes, an uncontrolled illness, does not affect your financial condition. It develops. Because the upfront cost of the antibiotic was prohibitive, a minor, treatable infection might turn into a disastrous hospitalization. The harsh arithmetic of poverty is this: a $50 prescription today against a $5,000 emergency room charge in a month.
The expense, however, is even more sinister. Uncontrolled illness and persistent pain deplete cognitive ability, focus, and energy—the very instruments needed to seek a better job, perform at work, or continue school. It turns into a trap. Your financial situation ensures the ongoing deterioration of your health; your health stops you from bettering your economic status. The decision between financial stability and health is a misguided one; in practice, you frequently lose both.
Can Community Care Networks Bridge the Gap Left by Traditional Medicine?
Getting medical care without health insurance calls for traversing a concealed, parallel system of care. Built on presumptions of flexibility, transportation, and discretionary income that simply don’t apply, the conventional healthcare model—scheduled appointments, specialist referrals, pharmacy runs—is grounded. True creativity is taking place in community-based ecosystems. This covers federal qualified health centers providing sliding-scale fees, but it goes further.
The monthly volunteer-staffed clinic is held at the local church. The non-profit collaborates with a major hospital network to offer pop-up diabetes screenings and education at the public library. The community health worker, usually from the area they serve, guides, translates, and advocates to help patients negotiate appointments, applications for support programs, and comprehend treatment plans. These networks go beyond care; they offer cultural and logistical expertise, therefore resolving the trust deficit that is as significant a barrier as the economic one.
Where Can We Find Hope in the Science of Resilience and Adaptation?
Damage cannot bring the story to an end. The body has a great capacity for healing when provided even the smallest help, even as it may wear down. Emerging resilience science reveals disproportionate advantages from little, consistent treatments. Regular, moderate exercise—like the daily walking commute of someone without a vehicle—can greatly enhance metabolic and mental health. From inexpensive mainstays like lentils and seasonal vegetables, the process of making a basic, shared meal helps both neurologically and nutritionally and strengthens social ties while giving a feeling of autonomy.
Even five minutes of concentrated breathing on a bus can help to control that hijacked stress-response system. This is about identifying and purposefully using the health-promoting habits already in place or readily merged within the limits of a limited budget, not about glamorous health. It’s about changing the issue from Why don’t they take care of themselves? How might we help the natural desire to heal that still exists under the most difficult conditions?
The debate on poverty and health has to go beyond coverage statistics and into the lived, biological reality of inequity. It calls for systematic answers that, as passionately as we argue over insurance costs, tackle housing, pay, and environmental justice. But it also calls for platforms that give voice to these difficult realities and for the boosting of stories and tactics highlighting human resiliency in low income health challenges.
Part of the bigger discussion is this investigation of the profound biological and economic linkages between health and poverty. www.ravoke.com seeks to encourage development. Through supporting patient stories and expert perspectives, Ravoke hopes to bring about significant improvement in health outcomes. Their upcoming original docuseries, Four Days, for example, illustrates the strength of making room for raw, expert-led dialogues on neglected health issues—a model that is urgently needed across the whole spectrum of healthcare, including the crucial problems affecting low-income populations.